Dynamic Five-Pillar Approach Recently, I posted a new announcement on LinkedIn about a new service offering. I am partnering with two amazing women in healthcare: Camille White, MD, MHA, Founder & CEO of CW Health Consulting, LLC and Adrianne Hudspeth, MHA, CPC, CCVTC, Founder & CEO of Comprehensive Coding and Compliance Solutions, LLC. We are teaming up to provide a truly innovative offering for venture capital (VC) companies: A 3-day accelerated teardown assessment to de-risk investment decisions. Through our process we help VCs make more informed decisions on whether or not to further invest in a digital health portfolio company and make recommendations on how to move that company into larger partnerships to expand access and maximize revenues. Interested and want to learn more? Schedule a 15-minute call with me here. "What are the guiding decisions that make venture capitalists (VC) invest in a digital health company? Sure, there are general investment criteria, a VC thesis, and market dynamics that guide the investment decisions. Our solutions guide VCs in making a prescriptive investment and understanding the key factors that enable success – 10x returns.
VC funding reached an all-time high of $21.6 Billion in 2020, and it is on track to skyrocket in 2021 to $40.8 Billion. With Ro, Teladoc, Alignment Healthcare, and Komodo Health lucrative announcements, which investor wouldn’t want to enter the innovative world of digital health investing? We offer investors a decisive evaluation tool to determine whether a digital health company is worth funding. According to the National Venture Capital Association, approximately 25% to 30% of venture-backed businesses fail, and according to Becker's Hospital Review, 98% of digital health startups fail. We will help you de-risk your current and potential investments to enable you to thrive in the $21.6 billion digital health funding environment. Digital health is complex, and now investors can be confident in their decisions by utilizing our services: We are a consortium of clinically oriented digital health consultants providing advisory services. We bring technological expertise, management consulting, and skilled clinical leadership together to help venture capital companies achieve financial returns from technology investments. Our holistic approach to digital health optimization includes technical solutions, stakeholder engagement and education, clinical workflow evaluation, and reporting capabilities to help companies prepare for and maximize revenue in the digital health ecosystem by focusing on long-term, high-growth potential. We evaluate companies by using a unique five-pillar connected care framework:
Get in touch!
1 Comment
This year I spent an enormous amount of time reflecting on health equity and racial justice following the protests against police brutality this summer. I looked at the parallels and how it related to the digital health and venture capital (VC) ecosystems. Naturally, I spoke to colleagues and reflected on the lack of Black representation in digital health: physicians, founders and stakeholders.
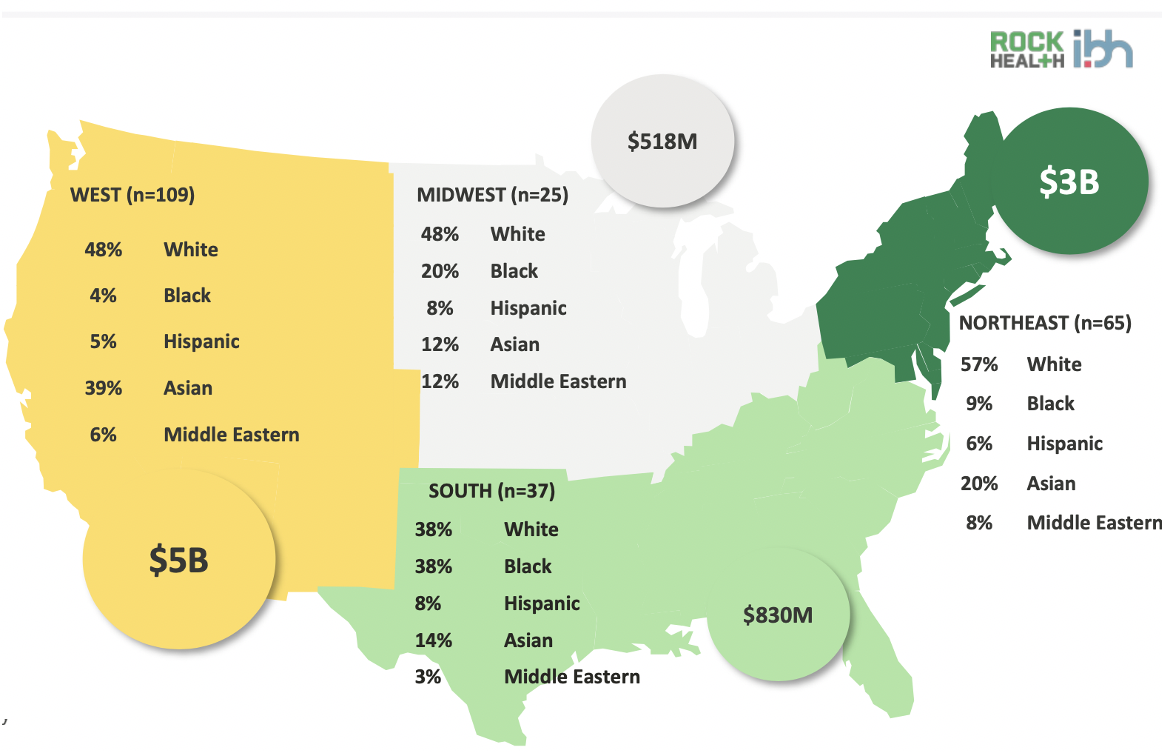
I reflected on times past, when friends would ask me, “Do you know any Black doctors?” They’d ask for my recommendations in specialties such as primary care, OB/GYN and dermatology. I realized a trend: it wasn’t easy to find Black doctors and it was more difficult to locate Black founders in the digital health ecosystem. Health plans and providers generally don’t list physicians by race. Digital health news and research outlets weren’t conducting extensive research on this issue. This past summer was the turning point for me. I was tired of the excuses, but what could I do about it? First, I set out to find Black founders of digital health companies. I searched the internet diligently, scouring several popular digital health and tech websites, followed by accelerators, incubators, and finally requesting referrals from colleagues at Columbia University Venture Community, Columbia University Black Alumni Council and Black Venture Institute (BVI). It was a project that kept me up at all hours, but I knew the outcome would be worthwhile. If I could identify Black founders and their companies, I could distribute the list, making it accessible to the public. Most importantly, this list represents companies and founders who are solving complicated problems and deserve more attention from the venture capital industry. This week, in BVI, Bill Gurley gave his thoughts on advancing diversity in the VC industry, he remarked that it was necessary to bring awareness and transparency to this significant subject and shine a light on success stories. The reasons behind the lack of representation in digital health are the same that I’ve heard in the tech industry: pipeline problems, networks, funding, education, etc. Fortunately, I know that Black people are resilient and pipeline problems have never stopped us from making waves in multiple industries. However, I also understand that sometimes the odds are stacked against us in the forms of bias and systemic racism. I’ve observed entire departments without a single Black physician and noticed partnerships being denied to Black companies, even if all their KPI’s outperformed the competition. This leads me to a recent study conducted by Rock Health and Dr. Ivor B. Horn. Their study highlights statistics that prove Black founders are receiving disproportionately less funding in the West, Northeast and Midwest regions. I was not surprised to find the South as a region where Black founders could thrive. Atlanta remains a strong hub for Black entrepreneurs in tech with support from government, HBCU’s, TechSquare Labs, Atlanta Tech Village and more. Source: Rock Health 2020 Diversity in Digital Health Survey, Rock Health Digital Health Venture Funding Database I believe problems are best solved by the people who live them. Black founders are uniquely positioned to solve some of the hardest problems in healthcare, because many of us have lived through the pain of a broken healthcare system and we’ve seen our loved ones die from preventative diseases such as cancer, diabetes and heart disease. I’ve been troubled by the unnecessary deaths and trauma inflicted upon Black women in childbirth. We can’t deny the disproportionate amount of death and sickness that has affected the Black community from Covid-19 exasperated by an inept administration. Additionally, in the VC industry, Black founders overall receive approximately 1 percent of funding. This problem of underrepresentation affects several layers of our tech and health ecosystems. Despite the odds, I remain optimistic and I am betting on Black founders. When I created The List, I was excited to see different challenges in analytics and clinical specialties being tackled: sleep science, maternity, chronic kidney disease, clinical trial analysis, drug drone delivery and more! I was even more thrilled to discover Black founders receiving millions in venture capital:
I also want Black founders to know that they’re not alone in digital health. There are over 70 companies on this list and most are funded with venture capital. In the tech ecosystem, I sometimes feel there is a lack of attention to healthcare, although that is changing. This is my effort to support Black founders and increase awareness of their companies in the digital health ecosystem. What's next? Deeper research and white papers on the ecosystem. Curated list of resources. Please contact me HERE if you identify changes that need to be made or if there is a company that isn’t present. I'd love to see this list continue to grow! By Tsahia Hobson for Tsahia & Company, LLC, providing strategic advisory services in value based care and empowered reimbursement for pre-seed and seed stage digital health startups, small businesses, local and federal governments. A special thank you to a few of my colleagues for being thought partners and helping me bring The List to life: @Dr. Camille White @LaAerial Owens @Narmeen Azad @Tesfa Wossne HBO’s Silicon Valley was one of the things that inspired me to come to San Francisco. When the show started, I was in the executive MBA program at Columbia University in New York. I was with my cohort for one long weekend per month over two fast-paced years, dreaming about Palo Alto, aka “Taxo Alto,” as they call it in the show. My curiosity was piqued watching the chaotic rise of Pied Piper, a tech startup. I became curious about venture capital (VC) firms and how their interest—or lack thereof—can spell life or death for startups. I loved Monica, the show’s VC, and her role dealing with the day-to-day responsibilities of the tech investment business and all its comedic wins and defeats. I started to attend tech and health care conferences. The best ones combined both topics and featured digital health technologies. My eyes lit up around VR/AR devices like OpticSurg a groundbreaking AR product transforming the surgeon operating experience, software that tracked heart disease, bodyweight scanners, and new apps that helped manage sleep and chronic conditions. I started locally by attending conferences at Columbia. Then I expanded my search and discovered health tech organizations in New York such as HITLAB, Brite, and Future of Care. As I learned more about health tech, listening to my professors and others at conferences, I developed my own interest in speaking to a larger audience. With my years of experience, I had a great deal to say. I saw that startups were interested in doing business with large organizations such as Columbia University Medical Center, where I worked in management for more than 10 years. I was a woman of color in health care management with a unique path that resonated with other women like me. After graduate school, I moved across the country to the San Francisco Bay Area and into a new industry: health insurance. People reached out to me to discuss both my recent relocation and my current work driving organizational innovation initiatives for Blue Shield of California. I decided to gain experience by becoming a panelist. I signed up for any opportunity I could find, as I was eager to contribute. After I had a few speaking engagements under my belt, I began to notice that there were things that could be improved. One was to have more information about the audience so that I could tailor my content. When I found out that I would be a panelist at Becker’s CIO conference in Chicago in the grand ballroom, I was thrilled. However, I remember imagining that my panel on women’s diversity and leadership in health care IT would be in a more intimate space. The grand ball room was reserved for CEOs, former presidents, and tennis stars like Venus Williams, who I would get to see at the conference. My visualization exercises did not include an audience that size, and I had to rethink how I would connect with the audience. Intimate venues have always been my preference, where I can look others in the eye, observe their body language, and gauge their interest. I remember thinking about what I was going to say. I did not have any questions from the moderator. All I could do was answer questions and tell my story with authenticity. The panel was amazing. These women gave out so many gems, and after the discussion, I was excited to see a line of women who wanted to speak with me to share their stories and hear more about mine. We were rushed because there’s usually very little time to move from one panel to the next. I would have liked to have more time with them as I enjoy one-on-one meetings with people to learn what inspires and motivates them. Answering questions one-on-one is great, but there should be an opportunity to take audience questions during presentations. This may not always work out for panel discussions, but it could be valuable for keynotes and speeches longer than 30 minutes. I always find that the audience asks the most intriguing questions. For example, when conducting research on a company, I often watch YouTube videos of the chief executives giving interviews. I remember one executive who was asked the same questions and gave the same answers over multiple interviews. It was not until audience members started asking unusual questions that this person became interesting again. I am certain that executives have a great deal more to say. Then there is the opposite type of presenter, the one who is so closely connected to her work that she wants to give the audience every single detail. It could be a new drug or device, or technical requirements and methods, and she forgets that the audience consists mainly of people who just want the headline and a bit of filler. They call this the “high-level overview” in the corporate world. This is why Silicon Valley’s Gilfoyle and Dinesh were never allowed to pitch to VC firms: they were too technical. Hilariously, in one scene, they gave away half of their company’s proprietary information during one presentation. In that episode, Gilfoyle and Dinesh were engaging only because the VCs wanted to steal Pied Piper’s data. It’s a useful lesson: gauge the audience’s interest early. The audience may seem disinterested, at least until the presentation is delivered in a way that is relatable. This is an excellent case for gathering real-time data from the audience during a presentation. 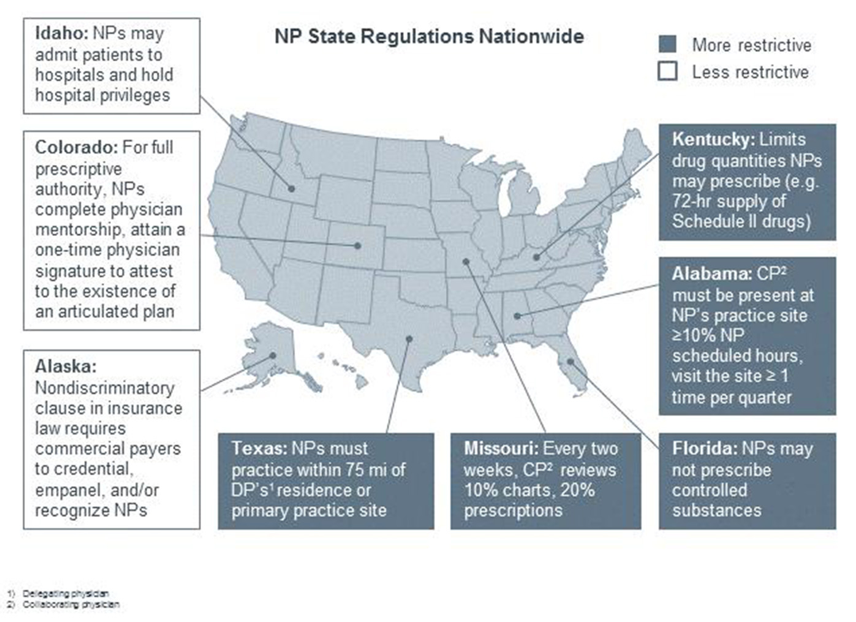 ABSTRACT Nurse Practitioners (NP) should be allowed to practice medicine independently without physician supervision because they are well qualified and suited to provide much-needed primary care, especially to residents in rural and underserved areas. The looming shortage of physicians, upward spiraling healthcare costs, the chronically ill and millions of newly insured by the Patient Protection Act (PPA) and the Affordable Care Act (ACA), have led to a surge in new NP led facilities. Currently 17 states allow NPs to practice independently; however, NPs are gaining legislative momentum as studies show patients are seeking high quality, low cost, accessible care. Still, organizations such as the American Medical Association (AMA) and American Academy of Physicians (AAFP) and other physician groups have vigorously opposed such autonomy. The Federal Trade Commission (FTC) has even had to step in to ensure that opposition is warranted and because not physicians and others with special interests want to thwart competition. BACKGROUND History and Overview - Nurse practitioners are the principal group of advanced practice nurses (APRN) delivering primary care in the United States and they are often the initial point of contact for patients in many settings.1 An APRN has completed coursework and clinical education beyond that required of the generalist registered nurse (RN). All NPs must complete a master’s or doctoral degree program and have advanced clinical training beyond their initial professional RN preparation. The NPs gain clinical competency and specialized knowledge through didactic and clinical courses, this training equips them to practice in a variety of health care settings.2 Advanced-practice RNs represent about 8 percent of the nursing workforce and encompass four distinct roles: nurse anesthetists, nurse-midwives, clinical nurse specialists (nurses with advanced knowledge and skills in the care of special patient populations based primarily in acute care settings), and NPs.1 According to the American Association of Nurse Practitioners (AANP), 89 percent of advanced practice RNs work in primary care- e.g. pediatrics, adult health, gerontology, or nurse midwifery. Of those in primary care approximately 49% specialize in family care. They provide high-quality care in all communities rural and urban and in various other types of settings, including hospitals, urgent care facilities, private offices, academic medical centers and military facilities.4 They diagnose and manage acute and chronic conditions, with an emphasis on disease prevention and holistic health promotion. 4 There are more than 192,000 NPs practicing in the United States, with a projected total of 224,000 by 20155 and they treat over 916 million patients per year.3 Today the NP educational curriculum has advanced to provide more comprehensive clinical training and now offers the “Doctor of Nursing Practice” (DNP)6 at several universities across the country. In the treatment of their patients, NPs collaborate with physicians and other medical professionals as needed. This lends a certain high level of trustworthiness to the system of the autonomous practice. The first NP program began in 1965 because of a projected physician shortage.7 Under the direction of President Lyndon Johnson, Medicare and Medicaid were enacted and provided access to high-level health care to Americans who did not have health insurance, or who were locked out because of access and affordability issues. Under the Patient Protection and Affordable Care Act an estimated 32 million Americans will be newly insured and ready to access new health services. 8 NPs are licensed in all states and the District of Columbia, and practice under the rules and regulations of the state in which they are licensed. However, they face many regulatory restrictions in other states because of restrictive scope of practice laws. See Map: 9 On trend with the growing demand for primary care services because of the growing baby boomer population, the rise in multiple chronic care conditions and the newly insured under the ACA, this paper discusses the contributions and benefits of nurse practitioners in primary care and why they should practice autonomously across the United States. Nurse practitioners as primary care providers “Nurse practitioners are experts in health promotion, disease prevention, health education, and counseling as well as the diagnosis and management of common, and complex, acute and chronic diseases.” 1 The ACA focus on shared-savings and incentives for preventive care and wellness benefits for people who are already insured – will increase demand for primary care services. To manage the growing demand, the ACA calls for the expansion of nurse led centers and to include more autonomy for nurse practitioners. 10 The current primary care shortage in the country is staggering. An Association of Medical Colleges (AAMC)11,48 led study predicts a physician shortage of 90,000. A 2009 study by the National Association of Community Health Centers (NACHC) placed the number of individuals “lacking access to primary care” at 60 million.12 In addition, only 9 percent of US medical students are choosing family and general medicine, the two primary care services where the need is greatest. 13 Nurse practitioners have been offering high-quality, cost-effective, patient-centered health care especially to the aging population and in rural and underserved areas. 3 The ACA expanded Medicaid coverage but has also enrolled many people in high deductible insurance plans. 14 Many physicians do not accept Medicaid plans because of low reimbursements;15 rates NPs have done the opposite. Eighty-nine percent of primary care nurse practitioners report treating children covered by Medicaid as their primary coverage and most NPs report that they are currently accepting new patients with Medicaid. (AANP) The vast majority of NPs treat patients between the ages of 66 and 85 years; and 79% treat patients older than 85, making NPs well experienced to treat an aging population.3 The Nurse Practitioner: Incredible Resource for the Health Care System The NP is an incredible resource in our health care system - NPs are more than just health care providers; they are mentors, professors, advocates, and administrators. Their involvement in professional organizations and participation in health policy activities at the local, state, national, and international levels helps to advance the role of the NP and ensure that professional standards are maintained. There is thus no question they contribute significantly to the intellectual development of the medical profession. Their focus on health wellness and prevention has been undervalued, but public health officials and others in the medical community are starting to value prevention over too much technology and acute-care driven services.20 Lower Healthcare Costs – By providing high-quality care and counseling by focusing on a patients “functional, emotional, spiritual and mental health,”21 NPs can lower the cost of health care for patients. For example, patients who see NPs as their primary care provider often have fewer emergency room visits, shorter hospital stays and lower medication costs. 22 As patients become more cost-conscious about their health care costs, 17 utilizing a nurse practitioner will become a comparable, if not preferred choice. Studies that compared insurance claims from nurse practitioners and physician costs and retail clinics, showed that lower costs were associated with NPs. 18 In a study by the RAND Corporation on behalf of Massachusetts, the average cost of a visit to a NP was 20-35 percent lower than the average cost of a physician visit. 19 By substituting nurse practitioner visits for physician visits the analysis estimated statewide savings of $4.2-$8.4 billion for the period of 2010 – 2020. 1 If the nurse-managed healthcare center can be expanded out of the niche of an academic medical center and low-income populations20, this can translate into significant savings across the country if NPs can practice independently. In addition, emergency rooms have been proven to be an overcrowded and expensive way in which to care of the urgent needs of patients, especially those with chronic and complex diseases. 6 Nearly 51 million uninsured Americans seek care in the ED for minor issues that are nonurgent 27,28 Clinics run by nurse practitioners create cost savings by reducing the need for emergency rooms and hospitalization. 28 Patient satisfaction and outcomes- In a 2013 survey conducted by the Pew Charitable Trusts, more than six in 10 Americans supported giving more autonomy to NPs and seven out of 10 opposed regulations that would limit the patients choice to choose a NP as a primary care clinician. 21 A survey released in Medscape22 found that only 50 percent of physician patients reported that they felt doctors “always” listened carefully, compared with more than 80 percent of NP patients. There is a growing body of research that shows patients who were seeing NPs were more satisfied, had longer consultations, and had appropriate tests, with no appreciable differences in patient outcomes, processes of care or resource use. 1 Nurse practitioners were found to perform better on measures of patient follow-up; consultation time; satisfaction; and the provision of screening, assessment, and counseling. What makes NPs Uniquely Qualified to Act in the Stead of Physicians in Certain Situations “Nurse practitioners also function as a combination of a patient educator and a social worker,” says Anne Norman, DNP, FNP – AVP of AANP. Given the training and practice of NPs, they fit comfortably in the niche between physician and RN. They deliver a unique blend of nursing and medical care. What also sets the NPs apart from other health care providers is their unique emphasis on the health and well being of the whole person-the holistic approach to health and well being. They tend to focus on health promotion, disease prevention, and health education and counseling, NPs guide patients in making smarter health and lifestyle choices, which in turn can lower patients' out-of-pocket costs. Thus, the NPs are invaluable in the goal of a healthier society, because of their focus on holistic health, prevention, and cost effectiveness. NPs also have distinguished themselves from other healthcare providers by focusing on the whole person when treating specific health problems and educating their patients on the effects those problems will have on them, their loved ones and their communities. By providing preventative care, high-quality care and counseling, NPs lower the cost of health care for patients. Patients who see NPs as their primary care provider often have fewer emergency room visits, shorter hospital stays, and lower medication costs.27 Women’s health NP’s are even credited with improving communities, “we address a major healthcare need because if women are educated about themselves and what they need to do to take care of themselves, the result is a better community.” 23 Barriers for Nurse Practitioners Scope of Practice – Each state has a regulatory board that defines the “scope of practice” of medicine22 and these laws are the most significant barrier to nurse practitioners being able to work independently in the United States. In 17 states including the District of Columbia, NPs can practice medicine autonomously. In other states, regulations can impose complex and time consuming supervision requirements. In some states such as Missouri, collaborating physicians must review 10% of NP-provided care services and 20% of their prescriptions- both on a biweekly basis. 24 In Alabama, the collaborating physician must be present at an NP's practice site for at least 10% of the NP's scheduled hours.9 Not only can this disrupt the physicians’ schedule, especially in hard to reach rural areas, but also it is completely duplicative and inefficient since the NP is providing the same care as the physician. In Georgia, NPs are required to practice within a specified distance of their collaborating physician. 9 California and Ohio prohibit NPs from admitting patients to the hospital, disrupting the continuum of care. 9 In Missouri, one of the most restrictive scope of practice states, the costs of regulations are “overwhelming” even though the ratio of NPs to physicians are 3:1 and NPs could be providing much needed care in the many rural areas of the state. 24 The most important consequence of these state specific restrictions is at a cost to patient care. With a greater need to coordinate care, especially for the aging population, those managing complex medication schedules and in rural and underserved areas; the most vulnerable are often more affected. It can also deter nurse practitioners from working in states with a higher need, but more restrictions. With the provisions under the ACA expanding the role of nursing, and large agencies such as the Robert Wood Foundation supporting autonomous practice, the federal government will surely have a “a compelling interest in the regulatory environment for health care professions . . . especially that of APRNs,” asserted by the IOM.25 Payer policies restrictions – The payment policies of commercial health plans, Medicaid and Medicare vary considerably. These health plans can choose not to recognize NPs as primary care providers regardless of whether or not the NPs are the primary care provider. Plans can also decline to credential or pay NPs, which significantly constrains their practice. Surprisingly, under Medicare NPs are unable to order home health care or durable medical equipment. However, in certified Rural Health Clinics in medically underserved areas, NPs are recognized as primary care providers and reimbursed at the same rates as physicians.26 In 2013, Aetna changed its policy regarding reimbursements and now reimburses NPs at 85 percent of the physician rate. 27 The hope is for payers and the federal government to follow suit and increase reimbursement rates. If NPs are to practice in stand alone clinics, they must be able to earn enough revenue to support the facilities, equipment, supplies, salaries, etc. Although there is progress, nearly one-fourth of major health maintenance organizations (HMO) do not recognize NPs as primary care providers. These credentialing policies could diminish the ability of NPs to provide care to the most vulnerable populations and allow the denial of care because of poor reimbursement rates or no reimbursement at all. 28 Even when state laws are relatively permissive, payers may restrict NP practice by offering NPs lower rates than physicians, reimbursing them for fewer services, and denying them status as primary providers and direct billers. Because there is so much variation in scope of practice across states, payers and decision makers can adopt, out of simplicity, the most restrictive of standards for payment. States should work with payers to remove these restrictions, highlighting NPs’ impact on quality improvement and cost reduction. Physician Relations In a survey of 972 clinicians (NPs and PCP) 29 physicians reported working longer hours, seeing more patients and earning higher incomes than did nurse practitioners. NPs were more likely than physicians to believe that they should lead medical homes, be allowed hospital-admitting privileges, and paid equally for the same clinical services. The majority of physicians agreed that they provide higher-quality examination and consultations than do NPs during the same type of primary care visit, 75.3% of NPs disagreed. Physicians and NPs do not agree on the quality of care they provide. The Council of Medical Specialty Societies (CMSS), representing 34 physician organizations and 650,000 US physicians, and the American Academy of Family Physicians (AAFP) strongly oppose allowing expanding the scope of practice for advanced practice registered nurses.30 Some physicians also cite a “lack of data” and “well-designed studies”31 as reasoning not to expand scope of practice. The AAFP believes that the effort to expand scope of practice for APRN comes at the same time when the medical profession is embracing patient-centered medical home and “changing to an integrated, team-based approach.” 30 In another survey of NPs and physicians29 the majority of physicians agreed that nurses should practice to the full extent of their education and training but physicians were less likely to agree (17.2% physicians vs. 82.2% of nurse practitioners) that NPs should lead medical homes or be paid equally for the same services (3.8% physicians vs. 64.3% of nurse practitioners). Despite these results, there is evidence of collaboration on the ground, but more dialogue, organizational support and patient focused collaboration are needed. 32 Gaps in the Research - The advanced practice nurse led center is not a new concept, but the research is not as robust as compared to physician led centers. As urgent care centers surge in communities across the US,12 and having the first clinician point of contact be a nurse – more research will need to be done in regards to care coordination, patient satisfaction, and patient outcomes. Since growing minorities of NPs also practice in subspecialty areas, it will be of great interest to evaluate outcomes in these type of clinics and the patient demand and market response. The impact on health care costs in local communities, states and across the country should be evaluated. Lastly, data will be needed to see if the public knowledge and awareness of the NP profession has increased and whether or not the public can differentiate between nurse practitioners and physicians. ANALYSIS To keep the population healthy and lower health care costs, policy makers and medical experts will need to work together to change the way health care is currently delivered. One solid option is to standardize the scope of practice and licensure laws for nurse practitioners, allowing them to practice autonomously in the United States. Nurse practitioners have been practicing medicine and receive scores of equal to better care from patients. The expansion of nurse run facilities, in a study conducted by the RAND Corporation, 19 states that the physician shortage can be cut in half by 2025 without training another physician. It also found that investments in technology coupled with better care coordination could totally eliminate the physician shortage. In New York, Columbia Advanced Practice Nurse Associates (CAPNA) is a full service NP led primary care clinic in Midtown Manhattan, where NPs are paid equivalent pay for equal service. Managed by Nursing Faculty from Columbia University, CAPNA focuses on an, “emphasis on individualized disease prevention and health promotion.” 33 Thanks in part to the recent passage for the New York State Nurse Practitioner Modernization Act, NPs are authorized to practice independently without a written collaborative agreement with a physician. 34 As states continue to deal with the primary care shortage, this law passed by NYS, a state with equally great rural and urban areas, will surely be a model going forward. Importantly, interpersonal working relationships between NPs and physicians need to be improved. Although, a majority of physicians support the IOM report on the future of nursing, which states NPs should be able to practice to the full extent of their education and training. A majority of physicians did not support equal pay for the same services, nurses being full partners with physicians and nurse-led patient care. The IOM’s report countered this, stating NPs should have hospital admitting privileges, reimbursed at the same rate as physicians for providing the same service.16 NPs have expanded from working in just primary care settings to specialty and subspecialty roles such as oncology, women’s health and diabetic care.5 Not many research studies offer any substantial reasons to not allow NPs to practice autonomously or state that NPs provide inadequate primary care. Most of the opposition comes from physician groups such as the AMA and American Academy of Family Physicians (AAFP) whose chairman, Dr. Roland Goetz stated the profession was worried it was losing control of the word “doctor.” 35-36.In response, the AMA launched a “truth in advertising” campaign to help patients distinguish the difference between a physician and a non-physician “doctor.” 37 Nurse practitioners and physicians do not have to compete; both can deliver quality care to patients and have a positive effect on patients. 38 CONCLUSION It is unlikely that a majority of physicians will soon embrace the standardization of nurse practitioners scope of practice laws across the country. However, policy experts and the ACA calls for changing the way in which medicine are delivered, focusing on patient care and patient centered medical homes. Graduate rates in nurse practitioner programs don’t show any slow down and advocates for primary care and the NP practice are persistently lobbying for standardization of these laws. Valid concerns exist whether or not NPs can be profitable in stand alone clinics if payers do not reimburse at sustainable rates. 41 Patients have agreed that that NPs deliver equivalent, if not better primary care than physicians and with the growth in retail clinics, especially led by major brands like CVS, Kaiser39 and Wal-Mart,40 and with a lower cost, patients will be encountering NPs frequently. It seems inevitable that the demand coupled with the high skill and holistic care provided by NPs, they would be able to achieve the gold standard in all states to practice independently. REFERENCES 1. Naylor MD, Kurtzman ET. The role of nurse practitioners in reinventing primary care. Health Aff (Millwood) 2010;29:893-9 2. "Nurse Practitioner Role in Family Care Partnership." Web. 11 Dec. 2014. <http://www.dhs.wisconsin.gov/ltcare/partners/infoseries/rs11-07.pdf>. 3. AANP – What’s an NP? American Association of Nurse Practitioners. N.p., n.d. Web 11 Dec. 2014 http://www.aanp.org/all-about-nps/what-is-an-np 4. 30. Morgan PA, Abbott DH, McNeil RB, Fisher DA. Characteristics of primary care office visits to nurse practitioners, physician assistants and physicians in the United States Veterans Health Administration facilities, 2005 to 2010: a retrospective crosssectional analysis. Human Resources for Health (http://www.human-resources-health.com/content/10/1/42). 5. Ruegg, T “A nurse practitioner-led urgent care center: meeting the needs of the patient with cancer.” Clin J Oncol Nurs. 2013 Aug 1;17(4):E52-7. doi: 10.1188/13.CJON.E52-E57. 6. "Breaking: Mundinger to Step down as School of Nursing Dean." Columbia Daily Spectator. Web. 11 Dec. 2014. <http://columbiaspectator.com/2009/03/27/breaking-mundinger-step-down-school-nursing-dean>. 7. Mitchell, Charles, and Robert Spinelli. "Medicare Reform and Primary Care Concerns for Future Physicians." The Journal of the American Osteopathic Association 113.10 (2013): 776-87. Web. 8. About the Law. Healthcare.gov. Accessed 1 Dec. 2014.. http://www.healthcare.gov/law/about/index.html 9. "A Guide to Understanding State Restrictions on NP Practice." The Advisory Board Company. N.p., n.d. Web. 11 Dec. 2014. 10. 42 U.S.C. 6A: Public Health Service. 11. American Association of Medical Colleges. (2012). Recent studies and reports on physician shortages in the U.S. Retrieved from https://www.aamc.org/download/100598/data 12. "The Case for Urgent Care." Http://www.ucaoa.org/. 1 Sept. 2011. Web. 1 Dec. 2014. 13. National Resident Matching Program www.nrmp.org 1 Dec. 2014. 14. Wharam, J. F., F. Zhang, B. E. Landon, S. B. Soumerai, and D. Ross-Degnan. "Low-Socioeconomic-Status Enrollees In High-Deductible Plans Reduced High-Severity Emergency Care." Health Affairs (2013): 1398-406. Print. 15. Ollove, Michael. "Are There Enough Doctors For The Newly Insured?" Kaiser Health News Are There Enough Doctors For The Newly Insured Comments. 3 Jan. 2014. Web. 11 Dec. 2014. <http://kaiserhealthnews.org/news/doctor-shortage-primary-care-specialist/>. 16. "The Future of Nursing: Leading Change, Advancing Health - Institute of Medicine." The Future of Nursing: Leading Change, Advancing Health - Institute of Medicine. 5 Oct. 2010. Web. 11 Dec. 2014. <http://www.iom.edu/Reports/2010/The-Future-of-Nursing-Leading-Change-Advancing-Health.aspx>. 17. Mehrotra A, Liu H, Adams JL, Wang MC, Lave JR, Thygeson NM, et al. Comparing costs and quality of care at retail clinics with that of other medical settings for 3 common illnesses. Ann Intern Med. 2009; 151(5):321–8 18. Thygeson, M., K. A. Van Vorst, M. V. Maciosek, and L. Solberg. "Use And Costs Of Care In Retail Clinics Versus Traditional Care Sites." Health Affairs 27.5 (2008): 1283-292. Web. 19. Eibner, E et al. (2009). Controlling Health Care Spending in Massachusetts: An Analysis of Options. RAND Health. 20. Coddington J. (2010) Quality of Care and Policy Barriers to Providing Health Care in a Pediatric Nurse-Managed Clinic. Journal of Pediatric Healthcare, 24 (5):e9 21. Vestal, Christine. "ACA Medicaid Expansion Hurts Physician Shortage, Empowers Nurses -- Stateline." 19 July 2013. Web. 11 Dec. 2014. <http://www.pewtrusts.org/en/research-and-analysis/blogs/stateline/2013/07/19/nurse-practitioners-slowly-gain-autonomy>. 22. Crane, Mark. "NPs Top Physicians in Small Patient Satisfaction Survey." Medscape Medical News. 27 July 2011. Web. 11 Dec. 2014. <http://www.medscape.com/viewarticle/745381>. 23. Fontenot, Holly, and Joellen W. Hawkins. "The Evolution of Specialists in Women's Health Care across the Lifespan: Women's Health Nurse Practitioners." Journal of the American Academy of Nurse Practitioners 23.6 (2011): 314-19. Web. 24. Kliethermes, Jill. "ADVANCED PRACTICE REGISTERED NURSES SCOPE OF PRACTICE IN MISSOURI." 1 Jan. 2012. Web. 12 Dec. 2014. <http://www.doctorsofnursingpractice.org/documents/2012KliethermesPPT.pdf>. 25. Iglehart, John K. "Expanding the Role of Advanced Nurse Practitioners — Risks and Rewards." New England Journal of Medicine 20.368 (2013): 1935-941. Print. 26. American Medical Association (AMA), AMA Scope of Practice Data Series: Nurse Practitioners, Chicago, Ill. (October 2009). 27. (APRNs a "Big Part of the Solution" to the Primary Care Provider Shortage - Robert Wood Johnson Foundation) 28. (Population Health Management 2013;16:306–309) 29. Donelan, Karen, Catherine M. Desroches, Robert S. Dittus, and Peter Buerhaus. "Perspectives of Physicians and Nurse Practitioners on Primary Care Practice." New England Journal of Medicine 368.20 (2013): 1898-906. Web. 30. "CMSS RESPONSE TO THE FUTURE OF NURSING REPORT." Web. 11 Dec. 2014. <http://www.cmss.org/uploadedFiles/Site/CMSS_Policies/IOM FON Report CMSS Response.pdf>. 31. Chen, Pauline. "The Gulf Between Doctors and Nurse Practitioners." The New York Times 27 June 2013. Web. 2 Dec. 2014. 32. How to foster interprofessional collaboration between physicians and nurses? Incorporating lessons learned in pursuing a consensus. Princeton, NJ: Robert Wood Johnson Foundation, January 2013. 33. CAPNA http://www.cumc.columbia.edu/patient-care/findhealthcare#sthash.5MqOWmeK.dpuf 34. "S6356D-2013 - NY Senate Open Legislation." Web. 11 Dec. 2014. <http://open.nysenate.gov/legislation/bill/s6356d-2013>. 35. 25. Harris G. Calling more nurses ‘doctors,’ a title physicians begrudge. New York Times. October 2, 2011:A1. 36. Beck, Melinda. "Battles Erupt Over Filling Doctors' Shoes." Wall Street Journal. 4 Feb. 2013. Web. 12 Dec. 2014. <http://www.wsj.com/articles/SB10001424127887323644904578271872578661246>. 37. Truth in advertising campaign. Chicago: American Medical Association, 2010. 38. Garment, Victoria. "Nurse Practitioners and Physician Assistants: Why You Should Hire One (or the Other)." The Profitable Practice Blog. 31 May 2013. Web. 3 Dec. 2014. <http://profitable-practice.softwareadvice.com/nurse-practitioners-and-physician-assistants-why-you-should-hire-one-or-the-other-0513/>. 39. Luthra, Shefali. "Win-Win? CVS Joining Forces With Hospitals, Doctors." Kaiser Health News WinWin CVS Joining Forces With Hospitals Doctors Comments. 24 Sept. 2014. Web. 11 Dec. 2014. <http://kaiserhealthnews.org/news/cvs-medstar-team-on-electronic-medical-records-coordination/>. 40. Appleby, Julie. "The Walmart Opportunity: Can Retailers Revamp Primary Care?" Kaiser Health News The Walmart Opportunity Can Retailers Revamp Primary Care Comments. 17 Nov. 2011. Web. 11 Dec. 2014. <http://kaiserhealthnews.org/news/walmart-opportunity-can-retailers-revamp-primary-care/>. 41. Auerbach, D. I., P. G. Chen, M. W. Friedberg, R. Reid, C. Lau, P. I. Buerhaus, and A. Mehrotra. "Nurse-Managed Health Centers And Patient-Centered Medical Homes Could Mitigate Expected Primary Care Physician Shortage." Health Affairs: 1933-941. Print. I've had a personal affection for Denmark since I was a baby, when my mother brought me there to visit her sister-in-law and my two cousins. I will have to dig up the baby pictures for another post! In 2008, I reconnected with my cousins in Copenhagen and have made several visits since. I also spent my vacations in Denmark talking to citizens about the Danish healthcare system and making comparisons it to the U.S. healthcare system. The Danish system, undergoing changes of its own and leaning towards more cost-sharing for individuals, is a system that provides healthcare for all. Denmark healthcare system focuses around primary care first and then specialists visits. The U.S. has caught on, realizing that so many conditions can be prevented, treated and managed by prioritizing primary care. I had given this presentation to strategy leaders at a major hospital in New York. I wanted to give them fresh perspective and inspiration by presenting some information on Innovisits and the Danish healthcare system. Although, there are distinct differences between our healthcare systems, we can be inspired and bring some (big and small) innovations back from Denmark. I must say that I have been enamored with this word, "Innovisit." I first heard it from Diane Stover-Hopkins, a panelist on the Innovation and Technology panel at the Becker's Annual Revenue Cycle and IT conference in Chicago about 2 years ago. I always knew what an innovisit was but had never heard the term until the conference. In graduate school, I studied the Virginia Mason case of implementing the Toyota Production System from Japan and the creation of Health City Cayman Islands (HCCI), a partnership between Ascension Health and Narayana Hospital in India. After doing some digging, I found an article from HBR highlighting steps to bring outside innovations into healthcare. This fascinated me and I became excited about the concept because so often we hear about the "silos" in healthcare. The silos run deep. So, how do we over come this? Check out my presentation and shoot me an email if you would like to discuss more.
I have been sitting in the office plugging away at my Q2 budget since 11am and it’s almost 2:45pm now. The budget is due in a week for initial review. I’ve wasted countless hours struggling to constantly reload my internet browsers to access the financial information stored in the recently installed cloud-based system. The system was meant to integrate the IT infrastructure and enable a collaborative information exchange among the hospital, insurers, and pharmacy systems. However, things have been slow since the hospital was forced to negotiate a new deal with its internet service provider (ISP). Frustrated, I look over at my phone and it says, “phone not recognized.” With my limited VOIP (voice over IP) knowledge, I plug out the cords and plug them back in. Now the phone says “Resetting” and it does this for about 10 minutes. While I wait for the phone to reset, anxious that it won’t work in time for my 3:30pm committee call with patient safety committee and clinical operations, I call the IT department to resolve the VOIP issue. I’m on hold for about 4 minutes and then IT transfers me over to Telecom. The rep asks me for my office phone number since I had to call from my cell phone. The telecom rep says, “you have departmental coverage for this service so call your department IT service.” Perplexed, I hang up and something is still wrong with my internet browser and the financial systems are still barely loading. I suppose the company that provides our financial systems is not a preferred choice for our telecom provider. Resolving to settle and take the conference call with my cell phone if the VOIP phone doesn’t work, I go back to finishing my analysis. John, the finance manager, comes into my office to tell me his phone isn’t working and the budget information is so slow to load and they’ll need an extension on my budget deadline, which impacts my overall budget. I take a deep breath and explain the urgency and ask if he can work offsite. “Maybe the Internet elsewhere is faster?” He is happy to work elsewhere with the possibility of faster internet and assures me he will try to get things done. Once I get to turn back to my work, my cell phone buzzes. I get a text that my old friend from high school has been admitted to the hospital. The hospital is in Des Moines, Iowa – the city where I grew up before leaving to NYC for college. I remember a few of the hospitals there, but I have to go online to search for hospitals. “Where could he be and why isn’t there an easy way to search for someone in the hospital?” I think to myself. The clock is ticking and it’s about 3:23pm, I have just enough time to search for and call a few hospitals. I search for hospitals in the zip code 50311 and call the first. The first person picks up and I tell her that I’m looking for someone and I’m transferred twice to the Emergency Department (ED). The ED nurse tells me that he’s not there. I ask, how many hospitals are in the area or what are the major ones? She says, oh there are several large ones in the area. I sigh, watch the clock and say “ok, thank you.” Now it’s 3:30pm and I have to jump on the conference call. I call my colleague and the phone goes straight to voicemail. I dial again in a few minutes but the phone goes straight to voicemail. I check my email, but there’s no message of postponement. Wait, it’s now about 3:40pm and I know my colleague has the same VOIP phone as me and maybe she’s experiencing the same problem. The VOIP phones were installed about two years ago to reduce costs. I just decide to walk over to the office, it contributes to my 10,000 steps per day challenge. Shoot, my cellphone service seems to work well but my apps aren’t quite syncing at the usual speed. Just as I start walking, Gina, the call center manager, texts me, “your phones in the practice are down and no one can get through!!” I know if the phones are down, the internet must be down. That means the doctors can’t access patient medical records, complete notes and submit entries for billing. It also means the front desk can’t check in/out patients, complete prior authorization requests, send e-referrals, set new appointments and other healthcare-intense online documentation. I text Cynthia, the practice manager, and ask her how she’s doing. She says, “everything’s fine.” I decide to skip the original meeting, figuring they’ve either not met at all or begun meeting without me. In the halls I pass Rashad, the administrator for Surgery. He looks like he’s seen a ghost. He tells me that patients and doctors are saying the telemedicine services are slow and choppy. He’s concerned about the remotely-monitored medical devices and the rural satellite clinics are slow and patient care may be impacted. I grit my teeth and tell him good luck because I need to attend to my own crisis. Then, I remember to call the next hospital on the list. The attendant says, “he’s here, let me transfer you to his nurse.” She places me on hold for 8 minutes and 43 seconds. At the same time, I observe the front desk staff in the practice trying to calm patients who have been waiting for hours. I’m still on hold waiting to be transferred and I exchange some conversation and strategy with the staff, while on hold. “Hello, this is the nurse, I can’t give you medical information, but he’s well enough to speak to him.” I speak to Thomas for two minutes and feel assured that all is well. I apologize to everyone in the practice for being on the phone and explain the situation. They forgive me and 15 seconds later, we jump into the chaos that has ensued as a consequence of the net neutrality repeal which led to slower choppier internet services. The hospital’s ISP was now able to charge the same rate for slower internet speed, especially since there were now only two providers in the area large enough to support the needs of this large organization. The service also provided less customer support and the IT and Telecom departments were stretched thin. However, the hospital faced costs of over $800 million for an EHR (electronic health records) implementation over the next few years and funding was just not available for the added expense for telecom... Fortunately, nothing in this story is true because the current net neutrality regulations have not been repealed. However, as a healthcare professional, I am deeply concerned regarding any slowing of the internet especially as it relates patient care. In healthcare, we rely on the internet for nearly everything we do: Telemedicine, Interoperability Requirements, Teaching, Revenue Cycle, Electronic Health Records, Medical Software Systems and Mobile Applications. Our patients, providers and staff deserve a healthcare system that is fast, responsive and reliable. I hope this fictional event has shed light on the seriousness of net neutrality and why we need it in healthcare. Do you agree or disagree with this scenario? Last week in San Francisco, my second favorite city (Copenhagen is my first), I attended the second annual AfroTech conference. AfroTech brought together influencers, change makers, entrepreneurs and techies from across the country to network and share experiences in the tech industry. This trip originally began as a visit to see friends, including two of my former classmates from the executive MHA program at Columbia University’s Mailman School of Public Health; however, it morphed into something much more magical.
I arrived in San Francisco on Wednesday, and on Thursday, I was with AfroTech attendees at the Kapor Center for Social Impact, hearing from venture capitalists (VCs) and inquiring about any new health ventures. Following the event, I co-hosted a public health happy hour at Dirty Water for Bay Area Mailman alumni with Vanessa Mason, co-founder of P2Health, a public health venture firm. The evening was a huge success and I was excited for the next two days of AfroTech, where I would hear from a host of VCs, entrepreneurs, policy makers and influencers. Some of the most influential companies were at the conference, including Johnson & Johnson, Twitter, Tinder, Facebook and Amazon. I was intrigued when speaking with people from these various tech companies, because I am constantly learning how other companies approach problem solving. In this way, I had the opportunity to conduct mini “innovisits” with these companies. Plus, I couldn’t contain my excitement from seeing J&J, the only healthcare company, and questioning the Amazon reps to find out what Jeff Bezos would do in healthcare. On the first day of AfroTech, Mandela SH Dixon, a startup veteran and one of the emcees, told us to have our “gem buckets” ready for all of the gems we’d drop in there. Since my birthstone is emerald, that has to be the best gemstone. I received an emerald from a J&J Vice President, who said (paraphrase) mentorship is good, but sponsorship is what you need. In my career, I made sure to always have mentoring, but I had not focused on sponsorship. Sponsorship is having a very senior person at your company who advocates for you and your career within the company. A sponsor is usually two to three levels above your position. Sponsorship is more transactional, because you need to identify clear goals for your sponsor to help you in growing your career. In a relationship based world, mentorship is not enough, we need sponsors to get us in front of the right people to further our careers. The Society from Human Resource Management (SHRM), reported that 30 percent of all hires overall in 2016 resulted from employee referrals and 45 percent resulted from internal hires. After thinking about what mentorship and sponsorship means for my career, I reflected on my own experience mentoring first year public health students at Mailman. They often come in for interview or career advice, which I am happy to deliver, but now I am thinking about the next level, going from mentorship to sponsorship. How can I sponsor someone in her career and truly create opportunities for growth, development and mobility? On the other hand, from the perspective of a seeking a sponsor, how can I: 1. Find a sponsor 2. Use her valuable time effectively and 3. Position myself for the career I want. Here are Tsahia's Top Five Steps: 1. Observe – your company’s leaders and take the time to determine the right fit. Look at least two to three levels above you. Be sure to choose sponsors who can push your career forward. Don’t just choose like-minded people, but choose those who can stretch and challenge you in your career. 2. Commit - to the process and do the work. In this phase, work on building trust. Neither mentors nor sponsors will commit to your success, unless you commit to the process and prove yourself. 3. Ask – and have specific goals. Don’t come to a sponsor as a jack of all trades. Let them know exactly what you want, so they can provide the right opportunities and assignments. Understand where your mission, vision and values are aligned. 4. Do - the work that’s required. You should have more than one sponsor, which means there will be a lot of work. There is nothing more frustrating than wasting someone's time. 5. Pay It Forward – and multiply the work of your sponsors. They aren’t in it for an ego boost. Sponsorship makes you look great but the work supports the company’s mission, work and succession planning. On Friday, February 24th, I attended the Columbia Business School's 13th Annual Healthcare Conference, "Shaping Healthcare's Future: Delivering Value Along the Continuum of Care." The conference featured some of the industry's top healthcare professionals from pharmaceuticals, managed care, consulting, government, technology and hospitals. The conference theme focused on delivering value, ultimately to the consumer.
The keynote speaker was Joaquin Duato, Executive Vice President & Worldwide Chairman, Pharmaceuticals, Johnson & Johnson. He spoke extensively on the benefits of medicine, how transformative medicine has been compared to any other industry and the role of the pharmaceutical industry in lowering costs and delivering value to the consumer. However, there is a tension between innovation and affordability when it costs between $3 - $7B to develop an approved drug and there is a level of uncertainty as it pertains to the administration's next steps. Mr. Duato's 5 Prescriptions for Controlling Healthcare Costs:
For the remainder of the day, I attended the following panels: Pharma's Next Act: Succeeding in a Value Based System; Sellers & Buyers: The Value Proposition of Digital Health; Fireside Chat: The Future of Healthcare Reform; and The $1 Trillion Idea: A Practicing Doctor & Healthcare Entrepreneur Tells US How to Really Fix Healthcare. These panels from the pharmaceutical industry gave me a new lens to view healthcare. Tsahia's Ten Takeaways:
When we move toward value, who wins? After reading a variety of news sources that predicted what might be next in healthcare for 2017, I decided to take a further dive into the specifics of the Republican healthcare proposals (RHCP). The next step in healthcare will likely include parts from Paul Ryan's "A Patients' Choice Act," Tom Price's "Empowering Patients First," the healthcare portion of the Republican's plan "A Better Way," and statements from President Trump.
One popular component of these plans is high-risk pools (HRPs). In this summary, I try to examine what it might mean for patients and the future state of healthcare. Regarding High-Risk Pools Prior to the Affordable Care Act (ACA), insurance policies sold on the individual market were medically underwritten. That means health insurance companies evaluated individuals' health status, health history and other risk factors such as pre-existing conditions, to determine price and coverage for policies. For example, a person with high blood pressure (HBP) on medication could purchase insurance on the individual market. However, the insurance would not cover conditions related to any illness that continued or developed from high blood pressure, since it was a pre-existing condition. Since the ACA took effect in 2014, health insurers have been prevented from denying medical coverage or charging unfairly high premiums to people with pre-existing health conditions. The effect has been that insurers are leaving the exchange markets and complaining that sicker people are buying plans and healthier people are not. This leaves insurers with the burden of not enough revenue to cover health costs. Specifically, an estimated 19 million "young invincibles" have not signed up for health insurance. To remedy the problems of insurers leaving the exchange market, stabilized insurance prices and increased access to affordable insurance for individuals and families, some conservatives and Republicans want to fund high risk pools. Their proposals include taking the sickest people out of the commercial market and putting them into "separate, tax-subsidized, high-risk plans." On the other hand, Dean Clancy, a former senior health policy advisor to congressional Republicans and the George W. Bush administration, called high-risk pools "targeted welfare." There are definitely mixed feelings on the matter by many people. For insurers and healthy people, the HRPs seem like a reasonable approach to stabilize health insurance prices. What is the cost? If the HRPs are not adequately funded and do not provide the health care that patients need, it will result in sicker people becoming even sicker, higher utilization of emergency rooms, health disparities and tax payers consistently footing an ever increasing healthcare bill. The Ryan plan proposes federal funding of $25 billion over 10 year while Price's plan proposes $1 billion over 3 years. Viability is a huge question regarding high risk pools. We have some historical data because some states have had or still have HRPs. A December 2014 Commonwealth Fund study concluded that the pools are:
In addition to the above, a small number of states limited enrollment in high-risk pools to control costs to the states. Even with limited enrollment, in 2011 net losses for 35 state high-risk pools were over $1.2 billion, or $5,510 per enrollee, on average. States financed these pools by revenue sources such as tobacco taxes and hospital assessments. Paul Ryan has proposed guaranteeing universal access to healthcare, but it's unclear how the government will pay for these high-risk pools. Health savings accounts (HSAs) have been part of the solution, but for high-risk pools with HSAs are not going to be nearly enough to help individuals and families cover medical expenses. To conclude, although we have historical data on what has happened with high-risk pools, some successful and some not so successful. Without knowing exactly who will make up these pools, how the pools will be funded and where the money will come from, I am not very optimistic about saying this option is better than a "Medicare for all" which insures everyone and spreads the risk in a practical way. As of December 2016, Republicans have not been clear on which of the current ACA tax/revenue streams they will repeal or keep. In a subsequent posting, I intend to continue discussion on this topic. One of the books I’m reading right now is called “The Other” by Wes Moore. It chronicles the story of two men with the same name, similar backgrounds, growing up fatherless in a Baltimore neighborhood. I was drawn to this story, because I often engage in discussions about “choice” and why some of us end up choosing the wrong path and how much empathy is deserved. In the book, How Will You Measure Your Life, (see summary here) my favorite section is “Staying Out of Jail.” The chapter begins with a quote from C.S. Lewis, “The safest road to Hell is the gradual one- the gentle slope, soft underfoot, without sudden turnings, without milestones, without signposts.”
Earlier today, I finally decided to answer one of those “No Caller ID” calls (the wrong path). My phone has been ringing off the hook with these calls. Just as I suspected, it was a democratic volunteer calling to ask me to donate into a fund to support gun control and background check legislation. Because I didn’t want to get up from the couch (NYC had a mini snow storm and I was feeling very cozy in the depths of my loveseat) to get my wallet, I told her that I didn’t have any money to donate (don't judge me). Then, she kindly persuaded me to give a reduced amount and told me some statistics about how many people are killed by gun violence in the US. The passion in her voice was convincing and she mentioned Gabby Giffords. I got up and donated… After the phone call, I started to think about Hadiya Pendleton, a special young woman whose life was tragically cut short on January 29, 2013. She was a 15-year-old girl from Chicago, Illinois who was shot and killed in a park, just after taking her final exams. Her story sparked national attention, even in the flurry of murders that happen in Chicago, because she had just performed at President Obama’s inauguration and First Lady Michelle Obama attended her funeral. There is a Facebook page dedicated to Hadiya, R.I.P Hadiya Pendleton with over 193K likes, a hashtag #wearorange to demonstrate against gun violence, and a foundation in her name, Hadiya's Promise, to inspire people to work for peace and put down guns. I often question why Hadiya's story resonated with me so much. Even now, I find this difficult to write. However, I realize that just like the similarities of the two men in Wes Moore's story, Hadiya's life was my own. When I was 15-years-old I lived in the midwest and attended Roosevelt High School in Des Moines, Iowa. I hung out with friends in the park after final exams, played sports, gave my parents a few headaches and enjoyed walking to Godfather's Pizza or Breugger's Bagels. Although, violent crime is not rampant in Des Moines like it is in Chicago, we know that violence can happen anywhere. Gun violence in the United States is a public health crisis, especially where children are concerned. According to the Brady Center to Prevent Gun Violence, 18,000 children and teens are injured or killed each year due to gun violence. In NYC, I rarely watch the local news because it used to depress me to hear about the constant acts of violence. Then, there are the national news stories: 9 yr old accidentally shoots her gun instructor, 1-year-old boy was accidentally shot by his sister, and 5-year-old accidentally shoots his 4-year-old brother... In addition to these tragedies are the mass shootings, from Sandy Hook to Charleston to Orlando. Many Americans, including me, thought that these horribly tragic events would spur our representatives to some sort of action, to finally come together in a nonpartisan way and create some legislation to help ensure these events would never happen again. I was quite surprised by the response from the NRA and others after Sandy Hook, and I knew then, this country had a long way to go before creating some commonsense reforms around gun violence. The AMA has recently adopted a policy on gun violence declaring it "a public health crisis," and will lobby to overturn legislation that prevents research in this area. But, this is not the first declaration of its kind. In 1993 the journal Health Affairs published an article on gun violence that stated, "The current epidemic of violence in America threatens not only our physical health but also the integrity of basic social institutions such as the family, the communities in which we live, and our health care system." In public health, we know there are many factors that spur gun violence. We also know we are a long way from preventing deaths due to gun violence and dealing effectively with the persistent impact this violence has had on our society. However, we can take action and support organizations like Hadiya's Promise and the Brady Center that are doing great work in the fight against gun violence. Peace |
Tsahia (like Tsunami - yes, the T is silent - Sa-hee-ah) is a healthcare enthusiast working to transform patient care for all of us while driving creative and innovative solutions with technology. Archives
March 2021
Categories |










 RSS Feed
RSS Feed